Whittier Health Network
Pulmonary Rehabilitation Therapy
Whittier Health Network provides Pulmonary Rehabilitation therapy at our accredited and certified acute rehabilitation hospitals. Our Bradford facility serves patients from the greater Boston and Merrimack Valley areas. Whittier Rehabilitation Hospital Westborough cares for patients in central Massachusetts.
What is Pulmonary Rehabilitation Therapy?
“Pulmonary rehabilitation uses supervised exercise, education, support, and behavioral intervention to improve how people with chronic lung disease function in daily life and enhance their quality of life.”
Restoring well-being and quality of life is the primary focus of Whittier Rehabilitation’s Respiratory Therapy Department. Our comprehensive pulmonary program offers high-quality treatment for various lung disorders and diseases. We’re honored that patients trust us on their journey to health and independence.
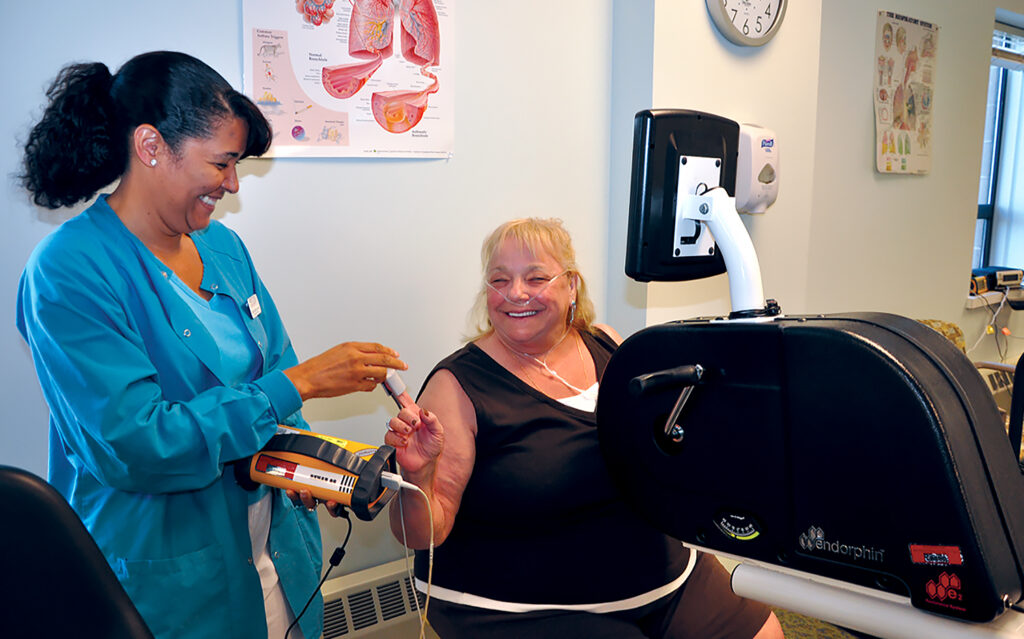 Whittier Rehabilitation Hospitals’ clinicians
Whittier Rehabilitation Hospitals’ clinicians
Our pulmonary rehabilitation therapists demonstrate their expertise and commitment to priority care for patients recovering from challenging health conditions. They specialize in assessing the cardio-respiratory status and administering medications. They recommend, acquire, and fit respiratory appliances. They educate and encourage clients and their families.
Whittier Rehabilitation Hospitals’ respiratory therapy clinicians work closely with pulmonologists to ensure patients receive only the best evidence-based treatments and therapies. Patients trust Whittier Rehabilitation when they need care for respiratory problems associated with pulmonary fibrosis, sarcoidosis, neuromuscular disease, COPD, COVID-19, lung cancer, cystic fibrosis, and many other diagnoses.
Pulmonary conditions
Obstructive pulmonary disease is characterized by problems exhaling all the air from the lungs. There are various symptoms, most commonly breathlessness, cough, and wheezing. Chronic obstructive pulmonary disease (COPD) includes asthma, emphysema, and bronchitis.
The lungs and ribcage lack adequate elasticity in restrictive pulmonary disease, becoming immobilized. Common causes are interstitial lung disease and scoliosis.
Goals of pulmonary rehab
Patients receiving pulmonary rehabilitation at Whittier benefit from 24-hour respiratory outpatient or inpatient therapy services. These specialists treat patients suffering from respiratory disease to decrease the number of acute hospitalizations due to exacerbations of the disease. Respiratory therapists improve patients’ quality of life by providing education and therapies to reduce shortness of breath as well as the anxiety and fear that breathlessness causes. Patients experience increased activity tolerance with pulmonary therapy.
Types of Pulmonary Function Tests
Also known as PFTs, “Pulmonary function tests measure the lungs’ capacity to hold air, move air in and out, and absorb oxygen.” These tests don’t diagnose diseases, but help evaluate and guide the best treatment for each patient’s needs.
These tests include:
- Spirometry: the most basic test to assess the amount of air breathed in and out
- Lung Volumes: uses a machine to see how much air the lungs accommodate
- Six-Minute Walk Test: evaluates the person’s ability to perform daily activities
- Cardiopulmonary Exercise Testing: uses a stationary bicycle or treadmill to evaluate breathlessness and identify decreased exercise tolerance
BiPAP, CPAP, ventilator, and tracheostomy care
BiPAP and CPAP are widely-used devices to support effective breathing in various circumstances.
BiPAP maintains two levels of pressure: inhalation and exhalation pressure, and it stands for bi-level (or biphasic) positive airway pressure. CPAP provides continuous positive airway pressure throughout both respiratory phases. Both devices keep the patient’s airway open, allow adequate oxygenation, and are often used to treat obstructive sleep apnea. The pulmonologist determines other therapeutic uses of PAP based on the patient’s diagnosis and needs.
Ventilator/Tracheostomy methods are more invasive compared to BiPAP/CPAP. For instance, the physician may need to introduce access through a tracheostomy. This surgical airway is covered with a special oxygen mask. Ventilators use BiPAP administered through a tube inserted through an oral airway. Patients are usually sedated while intubated to prevent vomiting, agitation, and anxiety.
Whittier can help patients reach their highest potential
Whittier Rehabilitation Hospital offers both inpatient and outpatient pulmonary rehabilitation programs. Let our experienced and dedicated staff of doctors, nurses, respiratory therapists, physical therapists, occupational therapists and speech language pathologists create a personal program to meet your specific pulmonary and respiratory needs. Our goal is to help our patients to reach their highest potential and to live productive lives within their communities.

